Periodontology: Healthy Gums for Healthy Teeth

Periodontology is an important branch of dentistry dedicated to the diagnosis and therapy of diseased gum tissue and bone surrounding the teeth. Periodontal disease left untreated can lead to bone destruction and premature tooth loss. Our practice is specialized in the treatment of periodontal disease. Dr. Schulte worked together with renowned periodontologists during his postgraduate studies and uses state-of-the-art techniques in his daily practice. We can offer our patients the complete spectrum of modern periodontal diagnosis and therapy:
- Prophylaxis and Dental Hygiene by highly qualified dental hygienists
- Bacteriological and genetic tests for the diagnosis of periodontal disease
- Gentle photodynamic laser treatment (DDT) for effective decontamination in the gum pockets
- Conservative periodontal therapy (Deep Scaling / Root Planing)
- “Full mouth disinfection” with aimed antibiotic therapy
- Probiotics for building up a natural oral flora
- Surgical periodontal therapy with guided bone and tissue regeneration techniques (GBR/GTR)
- Treatment of peri-implantitis (bone loss around dental implants)
- Surgical treatment of gum recessions and aesthetic correction of “gummy smile”
Read or print a complete article on one page: Periodontology
Topic overview:
Gum problems: from gingivitis to periodontitis
What Does Periodontal Disease (Periodontitis, Periodontosis) Mean?
Periodontal disease is normally a chronic, painless bacterial infection of the gums and other structures that surround and support the teeth (periodontal ligaments, bone). It is caused by different types of bacteria, some of them anaerobic, meaning they can live without oxygen.
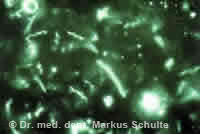
Bacteria from a gum pocket under the microscope
Our oral cavity is normally colonized by about 500 different types of bacteria, that, in small concentration, are easily controlled by our immune system. When oral hygiene is neglected, sticky plaques are formed, giving a base for multiplication of bacteria. Toxines produced by the bacteria cause inflammation of the gum tissue (gingivitis). This provokes bleeding of the tissue while brushing and flossing.
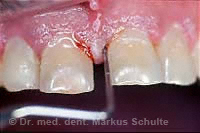
Gingivitis with pocket formation and bleeding on probing
If gingivitis is left untreated for a longer period of time, the infection will spread from the gum tissue to the supporting periodontal structures. It begins with pocketing of the gum tissue followed by bacterial colonization around the bone with subsequent bone loss.
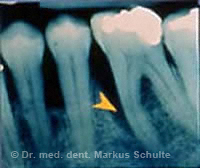
Advanced periodontal disease with deep bone pocket
Untreated periodontitis will lead to loosening and finally loss of the affected teeth.
Which Factors Favour Manifestation of Periodontal Disease?
- Inadequate oral hygiene: This is the most common cause of periodontal disease. Bacterial plaques lead to gingivitis and subsequent periodontitis. Above all, if other risk factors are present, oral hygiene plays a significant role.
- Smoking: Today it is a known fact that heavy smokers (more than 10 cigarettes per day) have a much higher risk of periodontal disease than non smokers. More, advancement of the disease is more aggressive and efficacy of treatment is reduced.
- Genetic disposition: It is an interesting fact that some people suffer from periodontal disease even though they have good oral hygiene, while others with poor oral hygiene present healthy tissue conditions. This phenomenon was a mistery for a long time. Today we know that about 30 per cent of the population have a genetic disposition to periodontal disease. With the ParoGen®-Test, we can easily test this genotype in our practice.
- Stress: Many studies show a connection between periodontitis and stress, due probably to stress-induced depression of the immune system
- Pregnancy: Massive hormonal fluctuation can create a pronounced tendency toward gingivitis and periodontitis.
- General illness: Above all, poorly regulated diabetes with high blood sugar level is a great risk factor for periodontal disease. Furthermore, certain forms of rheumatoid arthritis are considered risk factors, as are congenital and acquired immunodeficiency.
What are the Consequences of Periodontal Disease?
Here we have to distinguish between (1.) consequences for oral tissues and (2.) negative effects on the general health.
- 01. Recession of the gum tissue can create aesthetic problems, exposed root surfaces are susceptible to cavities and hypersensitivity. Mobile or migrating teeth or tooth loss are symptoms of an advanced periodontitis. Then, prosthetic treatment is often a problem because the remaining teeth are not stable enough to anchor a bridge or mobile prosthesis. Dental implants are frequently the only solution to maintain full chewing function.
- 02. Newest studies prove that patients suffering from periodontal disease have 2-3 times higher risk of heart attack and stroke. The cause was identified in anaerobic bacteria invading the blood stream from the periodontal pockets. It’s also known that pregnant women with pronounced periodontitis are eight times more likely to give birth prematurely or miscarriage.
How Can I recognise Periodontal Disease?
As the disease develops chronically and without pain, the early symptoms are not very characteristic. An important sign is gum bleeding on brushing and flossing, the first signal of gingivitis. Redness and swelling of the gums and bad breath can also be important symptoms. Loosening or migration of teeth is normally a sign of advanced periodontitis.
The proper diagnosis of periodontal disease can only be made by a dentist. Methods of choice are the periodontal chart and x-rays. The periodontal chart is virtually painless and done regularly with all patients in our practice. A calibrated perio probe is gently inserted between tooth and gum tissue at six different points around each tooth. With healthy gums the pocket depth is measured between 1-3 mm. Readings over 4 mm are suspicious for a more advanced stage of periodontal disease.
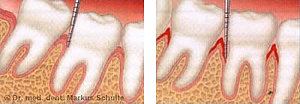
Measuring of the pockets left healthy, right pocketing
Periodontitis is treatable - but how?
The first phase of treatment (initial therapy) is to improve oral hygiene. The dental hygienist removes tartar and bacterial plaques, polishes the tooth surfaces and gives each patient an individual instruction to obtain optimal oral health. With good collaboration of the patient, this initial treatment should give pronounced improvement. If only the gum tissue is affected (gingivitis), the infection can be cured just by establishing correct oral hygiene.
Therapy: periodontitis is curable!
Deep Scaling and Root Planning
1-3 months later, a new perio chart is done and any further therapy is planned, if necessary. If deep pockets are still present, the next step will be “Deep Scaling”, meaning a deep cleaning of the subgingival root surfaces. Deep scaling cleans out these pockets and removes plaque and hard tartar from the tooth roots. This procedure is painlessly performed under local anaesthesia by the dental hygienist.
Antibiotics against Periodontal Disease
This new concept in fighting gum disease has become a more and more important part of treatment in the last years. This method is based on the fact that periodontitis originates from known types of bacteria which can be easily identified by a proper microbiological test.

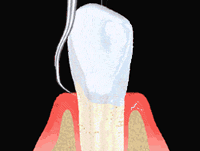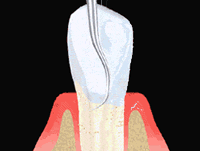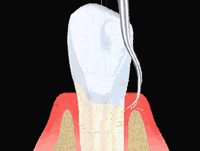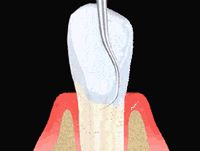
Sterile paper points are probed into the deep pockets for obtaining a bacterial sample and sent to a specialized laboratory. A few days later we receive a detailed analysis of the type and concentration of the bacteria colonizing the pockets.
Now we are able to choose an antibiotic that works specifically against the bacteria identified.
According to the result, a combination therapy with two different antibiotics can be necessary to optimize the efficacy. The antibiotics are taken in tablet form for 1-2 weeks and normally well tolerated.
New studies show a high success rate when periodontal disease is treated at the same time with antibiotics and curettage of the pockets. In many cases a permanent elimination of the aggressive germs can be achieved resulting in healthy gum tissue and periodontal structures.
Probiotics: Good bacteria fight bad periodontitis germs
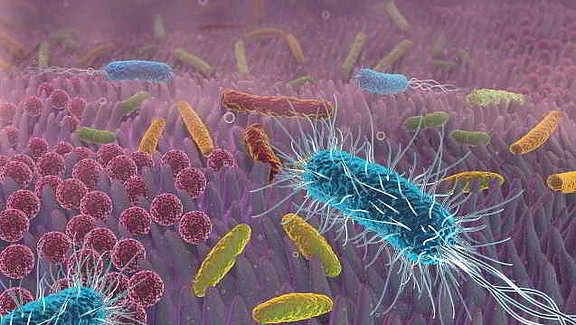
All mucous membranes in our body represent a possible gateway for pathogenic germs. This is particularly true for the outwardly exposed oral cavity. The protection of the body against such attacks is the thick layer of mucus, which is a barrier that is difficult to penetrate. It enables numerous harmless or useful microorganisms to settle, which act as “placeholders” and make it difficult for harmful bacteria to penetrate. These harmful microorganisms, e.g. the aggressive bacteria causing periodontitis, are always present in the oral cavity even under normal conditions, but are kept in check by the natural protective function of the mucous membrane. If this protective layer is no longer intact, pathogens can increasingly establish themselves and multiply. A strong inflammatory reaction then leads to the typical symptoms of periodontitis, which, if left untreated, lead to bone and tooth loss.
Probiotics are concentrates of natural, beneficial bacteria, such as lactic acid bacteria, which are often sold in the form of lozenges. Scientific studies have shown that by supplying such “good” germs it is possible to suppress “bad” bacteria and restore the natural balance. It could be proven that probiotics have a positive influence on the course of periodontal diseases. The gentle, biological treatment method with probiotics is therefore an ideal addition to the other therapies against periodontitis presented here.
Genetic Testing
Why are there patients with good oral hygiene suffering from periodontal disease, while others have healthy periodontal structures in spite of massive amounts of tartar? Why does periodontal disease occur more frequently in some families? Today, finally there is a scientific answer to these questions.
About 30% of the population has a genetic disposition and much higher risk to suffer from periodontitis. With the ParoGen®Test, a painless swab of the oral mucosa, we are now able to easily identify these patients that are considered high-risk patients and need specific control and maintenance programs. Perfect oral hygiene is mandatory for these patients, as is the avoidance of other risk factors such as smoking.
Photodynamic Laser Therapy (PDT)
A promising new approach to combat periodontal disease is the Photodynamic Therapy (PDT), which is also called Photodynamic Antibacterial Chemoterapy (PACT). A special light-sensitive dye is administered into the periodontal pockets to be irradiated with a soft laser, whose wavelength (635 nm) is optimally matched to the dye. The energy of the laser light is absorbed by the dye and the energetically excited dye passes its energy to oxygen atoms, which are thereby converted into the active singlet state. Singlet oxygen destroys the cell walls of bacteria, thus killing them. The healthy cells of the periodontal tissue remain intact. With this completely painless method it is possible to kill in a few minutes up to 99% of the germs causing periodontitis.
For a lasting effect, the PDT should be used only after mechanical cleaning of the periodontal pockets. It will therefore be applied following the “Deep Scaling” (deep cleaning), in which the subgingival tartar and bacteria-containing concretions are removed. The PDT can also be easily combined with the administration of antibiotics.
The advantages of photodynamic laser therapy (PDT/PACT):
- Non-invasive, painless and time-saving method, no anesthesia required
- Secure destruction of periodontal bacteria
- No damage to healthy tissue
- No possible development of resistance of the bacteria as with antibiotics
- Less use of antibiotics required
- Makes surgical treatments superflous in many cases
- Inexpensive compared to surgical procedures
- No side effects
We are pleased to offer our periodontitis patients this innovative therapy. The PACT laser we use is a diode laser of the latest generation whose wavelength is specially matched to the dye, thus ensuring optimum effectiveness.
More Information on Laser Dentistry
Surgical Periodontal Therapy
Until a few years ago, invasive surgical therapy was standard treatment for periodontal disease. Today surgical therapy is the option only after all conservative methods (hygiene pretreatment, scaling and root planning)have been performed and deep pockets still remain.
The aim of surgical intervention is scaling and planning of the contaminated root surfaces under direct vision to remove hidden tartar and bacteria from the bone pockets. With modern techniques such as Guided Bone Regeneration (GBR) and Guided Tissue Regeneration (GTR), it is now possible not only to stop periodontal disease, but also to regenerate lost bone and periodontal tissue.
The bone craters are filled with a bone substitute and covered with resorbable membranes. Protected by the membrane, the bone substitute is incorporated in one’s own bone.
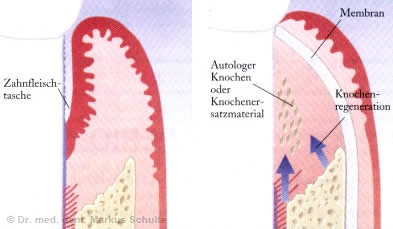
Emdogain: Growth Factors for Bone Regeneration
Another option for periodontal regeneration is the use of growth factors. After root planning, a gel consisting of bioactive growth-factor proteins (Emdogain) is applied to the surgical site. The growth factors induce the regeneration of bone and periodontal tissues.
Both regenerative techniques, GBR / GTR and Emdogain, are scientifically well-documented and regularly used in our practice.
Periodontal surgery is usually performed without pain using local anaesthesia. For anxious patients, sedation with nitrous oxide or other sedatives can be helpful.
Follow-Up and Maintenance
After the active treatment phase, the patient remains in regular maintenance visits with the dental hygienist. Depending on severity of disease, oral hygiene and periodontal resistance, the interval of recall appointments can range between 2 – 6 months. Long term studies prove that professional care and supervision is the key to maintaining positive results of periodontal treatment.
In our practice all patients are controlled with regular recall appointments, current perio charts, and individual dental hygiene instruction.
More information on preventive treatment.
Mucogingival Surgery
Gum recession
An attractive smile is the harmonious composition of teeth and gums. Gingival recession, e.g. as a result of periodontal disease, can lead to a significant deterioration of the cosmetic appearance. Gum or gingival recession(receding gum) is favored by particularly thin, sensitive gum tissue and is often caused by incorrectly brushing your teeth with brushes that are too hard. In contrast to periodontitis, the recession is not caused by inflammation. If necessary, the recession is treated by microsurgical gum reconstruction with and without gum transplants. Such a gum augmentation is necessary when
- The recessions lead to hypersensitive tooth necks
- The receding gums lead to inflammation and impaired oral hygiene
- The recessions lead to aesthetic problems
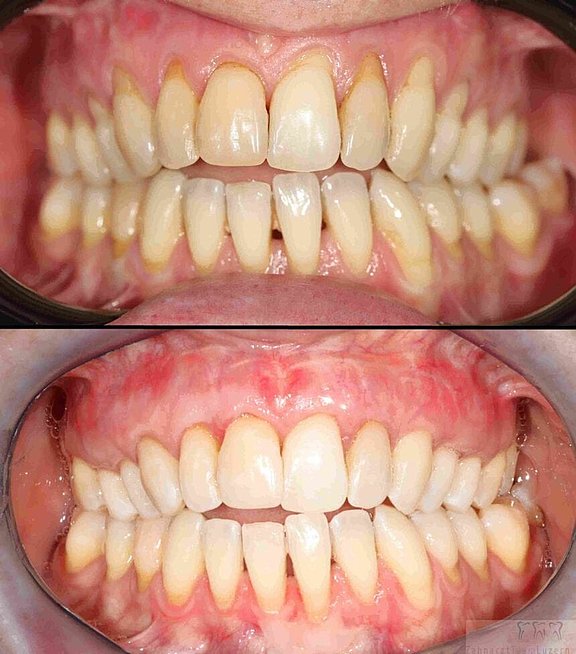
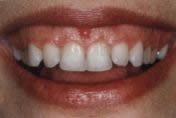
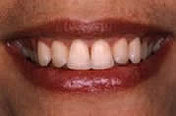
This 43-year-old female patient complained of receding gums on almost all teeth in the upper jaw (picture above), which she found aesthetically unpleasing and had already led to very sensitive tooth necks. In the picture below we see the patient three months after complete gum reconstruction with a gum transplant from the palate. Through this treatment, executed in one single surgery, we were able to permanently fix her problems.
Gummy smile correction
With “gummy smile”, the patient shows a disproportionate amount of gum tissue when smiling, which is often perceived as aesthetically disturbing. Several causes are possible: The gums often cover too large a proportion of the tooth crowns and make them appear too short. Sometimes the upper lip is too short or the middle face is too long. In many cases, aesthetic periodontal surgery can help. In mild cases of gummy smile, the excess tissue is gently and painlessly removed with the laser and a harmonious tooth shape is restored. When more tissue needs to be removed, minor surgery is sometimes required to optimally shape the bone under the gums.
If the gummy smile is caused by a hypermobile upper lip (which moves too far upwards), a surgical intervention can sometimes help in which the muscle attachment of the lip is detached and mobility is restricted (lip repositioning).
Gummy smile before and after microsurgical crown lengthening using the laser
Gingival mask
Sometimes periodontitis and bone degeneration is so advanced that surgical reconstruction of the lost tissue is no longer possible. Often these defects result not only in an aesthetic impairment but also a phonetic problem. The only solution for large gingival defects is a gingival mask. After an impression is taken, the laboratory creates an extremely thin gingival coloured resin mask that adheres perfectly to the teeth. This removable piece dramatically improves aesthetics and phonetics and fits comfortably for the patient.
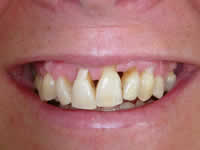
Left: This patient, after a recovery from periodontal disease, has severe gingival defects in the visible front teeth area. She feels uncomfortable with her compromised appearance.
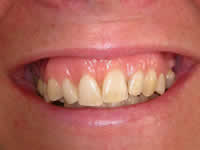
Right: By placing a gingival mask, we have reached an aesthetic reconstruction that satisfies the patient.
The alternative: New fixed teeth on implants
In particularly severe cases of periodontitis with considerable bone and gum loss and a poor prognosis for the affected teeth, it is sometimes better to remove them in good time in order to preserve as much jawbone as possible. Modern implantology makes possible a functional and aesthetic rehabilitation with fixed implant-supported dentures.
49-year-old patient with severe periodontal disease. Due to the massive aesthetic and functional problems, a total reconstruction was carried out: All teeth in the upper jaw were removed and replaced with a fixed all-on-four bridge on implants. In the lower jaw we were able to preserve the teeth with a periodontal treatment.
Questions and answers about Periodontal Disease
Contrary to cavities, periodontal disease doesn’t hurt. Frequently there are signs like gum bleeding. But not in all cases is this a reliable symptom. Heavy smokers, for example, have reduced blood circulation in their oral mucosa. So it is possible they have periodontitis without significant bleeding. Periodontitis can become painful when it is severely advanced and causes abscesses in the tissue. Furthermore, loose teeth can hurt with biting pressure.
Periodontitis always causes destruction of periodontal structures including bone, fibres and gum tissue. Due to the hypertrophy of inflamed tissue, however, the destructive process can remain hidden for a long time. That’s why regular perio charting and x-ray control are so important.
All periodontal treatments, from the initial dental hygiene to the surgical therapy, are absolutely painless using local anaesthesia. Thanks to modern technology, such as laser, today in many cases we can avoid surgery. For anxious patients, all kind of treatment can be done using conscious sedation with nitrous oxide.
In Switzerland, compulsory health insurance only covers dental treatment if the illness is congenital or unavoidable. Only in special and very rare cases of juvenile periodontitis in children and young adults, cost of treatment is reimbursed. All other forms of periodontal disease are excluded from coverage.
Thanks to modern diagnosis and therapy methods, in most cases the destructive process of periodontal disease can be stopped.
Over 80% of all cases of halitosis (mouth odour) have an origin in the oral cavity. Periodontal disease plays an important role because the bacterial composition of proteins in the pockets release bad smelling gases. Therefore, patients suffering from halitosis should first see their dentist.

